WARNING: The content shared may be graphic and discuss bodily functions with or without images. Do not proceed if this will offend you or you are not interested.
After leaving the hospital, Thanksgiving festivities, and recovery (my organs felt beat up for about a full week), the search for the cause of my hospital stay began.
December 2018 & January 2019
Throughout December and January, I started having some crazy weird gut issues that I had never experienced before. Sure, I may have had a bad meal, experienced a change in bowels for a day, but nothing like this ever before. These included the following:
- Constipation
- Diarrhea
- Terrible tummy cramps
- My stomach was making loud noises all the time.
- My colon would “talk to me” both while I was on and off of the toilet. It sounds funny to say, but that is the best way to describe it.
- I had pains off and on from both sides of my abdomen.
- Goosebump like strange feeling on my left thigh that would come and go, and never hurt but felt strange.
- I would feel an ache in the back of both thighs.
- At one point, I was in Costco and I had a stabbing pain in my back on the left side almost behind my rib cage that took my breath away. I had to lean on a rack I was walking by almost feeling like I was going to pass out and it scared the crap out of me.
- Shooting pains from my left side up through my right shoulder and down my right arm.
December 2018 Search for Answers – Still no answers
Despite 3 doctor’s office visits, I still had no answers.
- I had a follow-up with USF Internal Medicine. They instructed me to check with gyno on follow up and if gyno doesn’t have any answers, then I should come back. They didn’t know if my hospital stay, infection, etc. was caused by GI or OBGYN issues.
- I had a follow-up with USF gynecology. They encouraged me to look at going to a urogynecologist due to my prior interstitial cystitis. They also recommended that I look into Myofascial Pelvic Pain Syndrome. After a 3-hour office visit, they wanted me to come back in a few months for an ultrasound or scan of some sort. I decided to go to my gynecologist who I had seen prior for their opinion.
- I saw my gynecologist. She did an exam and did not feel the cyst that was present in the hospital ER reports. She wanted me to come back in January during my monthly cycle for a sonogram to see if the cyst was in fact there. It was at this point, that I learned that there are 2 kinds of cysts we were looking for/at:
- Simple Cysts: normal cysts that come and go with our cycle. This would not be present during a cycle (if I understood correctly).
- Complex Cysts: abnormal cysts that usually are filled with an endometrial substance that typically need surgically removed This would be present during my cycle as it continues to grow regardless of the cycle (if I understood correctly).
January 2019 Search for Answers – I probably have endometriosis
Gynecologist
I went to my gynecologist in January 2019 for a sonogram during my cycle as she requested. Of course, I was hoping that they would not find a cyst.
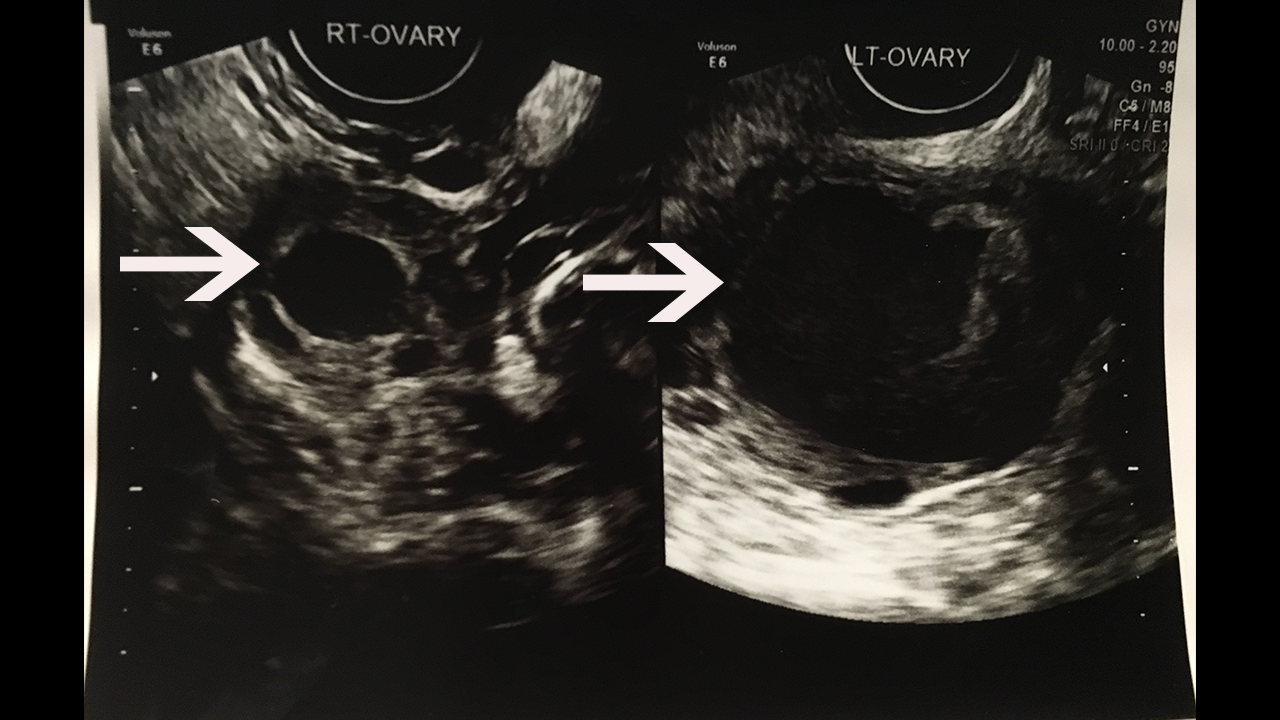
They located what appeared to be the exact same cyst that was located during my hospital visit. It had grown. It was 5cm x 3cm in November based on hospital records and now in November 2019, it was 5.3cm x 3.9cm. IT WAS GROWING!!!!

The right ovary is the small oval egg looking shape on the left side of the image.
The left ovary is the huge grapefruit looking shape on the right side of the image.
My gynecologist wanted to put me on the pill to “control my pain during my cycle” but the I was used to the pain during my cycle. It was no different than prior my hospital stay, so why would I go on the pill and put a chemical into my body to help with something I already can manage and is not the end of the world?
My doctor explained that it appears that I have a complex cyst, most likely an endometrioma caused by endometriosis. The sonogram tech and doctor said that the sonogram scan points to endometriosis, but it can’t be diagnosed without surgery. I refused birth control and decided to do my own research for holistic remedies. My gynecologist wanted me to return in April during my cycle to check the size of it at that time.
GI Doctor
Because I still didn’t have answers, I knew I needed to try to rule out GI issues so I went to see a gastroenterologist. After my consultation, they were convinced that I had Crohn’s disease and or possibly celiac. They wanted to conduct a colonoscopy and blood work.
Initially, I was on board, until I learned that a colonoscopy basically was an operation and I would have to be put to sleep somewhat for it. I opted to do the blood testing first which would show signs of Crohn’s or celiac and if the results warranted, then AND ONLY THEN would I follow through with a full colonoscopy.
The blood work revealed no signs of Crohn’s or celiac so my GI doctor agreed that there was no reason to move forward with a colonoscopy.
Nutritionist & Whole 30
I started taking some vitamins from Invite Health. I took some probiotics and digestive enzymes. I noticed a huge change in my gut functioning and discomfort after taking vitamins and eating a Whole 30 diet for 21 days.
Feb, March, April 2019 Still searching but looks like endometriosis
Functional Health Coach
By February, my GI issues were so much better. I still was having minor issues, but nothing like I had in December and January. I started working with a functional health coach online. They looked over my blood work and helped me see some areas of deficiency that I could improve with the use of targeted supplementation.
I started taking B12, Zinc, Enzymes, Probiotics, etc. I learned the importance of the type of vitamins that I need to take.
- I learned that it is beneficial to switch up the type of probiotic I take after running out of one. It is good to let your gut get different strains of different probiotics rather than always taking the same ones for months at a time.
- I learned that the dosage or milligrams are important.
- I learned that for most people it is advantageous to target certain types of vitamin supplements rather than just taking a multivitamin. A multivitamin typically has such a small portion of each type of vitamin that it is seldom as beneficial as taking individual specialized vitamins for a purpose.
- I learned the importance of the forms of some types of vitamins needing to be a mythl form for your body to absorb based on certain conditions in the body.
Conclusion Starting To Form
Due to my improvements with vitamins and diet, I was becoming more and more convinced that my IBS and GI issues were probably an effect of my supposed endometriosis and I no longer needed to see a GI doctor.
Continue to Part 3: Research Done & Surgery Scheduled!